TCA, vol. 20: A new fungus on the scene
Candida auris is a new human pathogen with possible ties to climate change.
In what seems to be a new chapter in the sci-fi story “The Last of Us”, a new fungus has emerged as a human pathogen. Candida auris has hit the news cycle lately, and for good reason. This new human pathogen has some troubling characteristics, but so far, only seems to infect those with compromised immune systems or severe underlying medical conditions.
What is C. auris?
C. auris is a yeast-like fungus in the same family as Candida albicans, which is a normal resident of the human body and is the cause of “yeast infections” when it overgrows. C. auris can grow on the human body without causing disease (colonizing the skin, ear canal, respiratory system) and can also cause invasive dangerous infections (bloodstream, internal organs, central nervous system).
How do you get infected?
Almost all human infections so far have been associated with hospitals or long-term care facilities like nursing homes. Most likely, it is transmitted by being touched by someone who is colonized or by contact with contaminated equipment or surfaces. Therefore, good hand hygeine and cleaning of surfaces is critical to prevention.
Who is at-risk?
Those who are immunocompromised or have severe underlying medical conditions and have frequent or prolonged stays in a medical facility. Others at risk are those with catheters or similar lines in the body, and those who have been on long term antibiotics or antifungal medications.
Healthy people are not considered at-risk.
Why is C. auris a problem?
C. auris does not cause any more damage to the body than its cousin, C. albicans (commonly called a “yeast infection”). But unlike C. albicans, C. auris is multi-drug resistant and so it is much more difficult to treat with the available anti-fungal medicines. Most C. auris infections are resistant to the standard anti-fungals like fluconazole and triazoles. Drugs like amphotericinB may be useful, but they can have dangerous side effects. One class of drug, echinocandins, seems to still work. However, strains of C. auris that are resistant to echinocandins are emerging.
Because we are losing the ability to control the growth of C. auris, infections can quickly become deadly in those who have compromised immune systems. It is thought that one possible reason why C. auris is so drug resistant is because of our overuse of anti-fungal drugs (like azoles) in the agricultural industry.
Another issue is that C. auris can be difficult to identify in lab samples, delaying diagnosis and treatment.
Invasive infections with C. auris has a mortality rate of 30-60%, although those who have died also have had severe underlying medical issues.
Where did C. auris come from all of a sudden?
So here’s the really interesting part of the story. C. auris emerged simultaneously in four locations (South Asia, East Asia, Africa and South America). It’s not known exactly how, but the thought is that C. auris was an unknown environmental bug and recently evolved to become a human pathogen.
In 2009, this new fungus was found in the ear of a Japanese woman (leading to its name “auris” meaning “of the ear”). It wasn’t associated with disease until 2011, in several cases in South Korea. Studies of stored human samples indicate that this fungus may have been colonizing humans as early as 1996. Within the last decade though, it has rapidly been identified in multiple continents and spreading through hospital systems.
Mammals are protected from severe fungal infections by two things: our immune systems and our high body temperature. When either of these two things fail, we are more susceptible to invasive fungal infections. This is commonly seen in immunocompromised people like those with advanced AIDS. In terms of temperature, most fungi are “mesophiles”, or organisms that grow at ambient temperatures like in the 70-80s Fahrenheit. Our hot 98 degree bodies are just inhospitable to them, especially on the warmest places like our internal organs. Places like our skin are a little more tolerable since they are a few degrees cooler.
Alarmingly, C. auris seems to be evolving to grow in warmer temperatures. Mutations have been identified in their Heat Shock Proteins, proteins that keep a cell from being damaged by high temperatures. It seems as if this fungus is growing to like warmer temperatures, maybe due to adaptations to climate change. These adaptations are making our warm bodies less of a danger. So, if your immune system also fails, then you are completely susceptible.
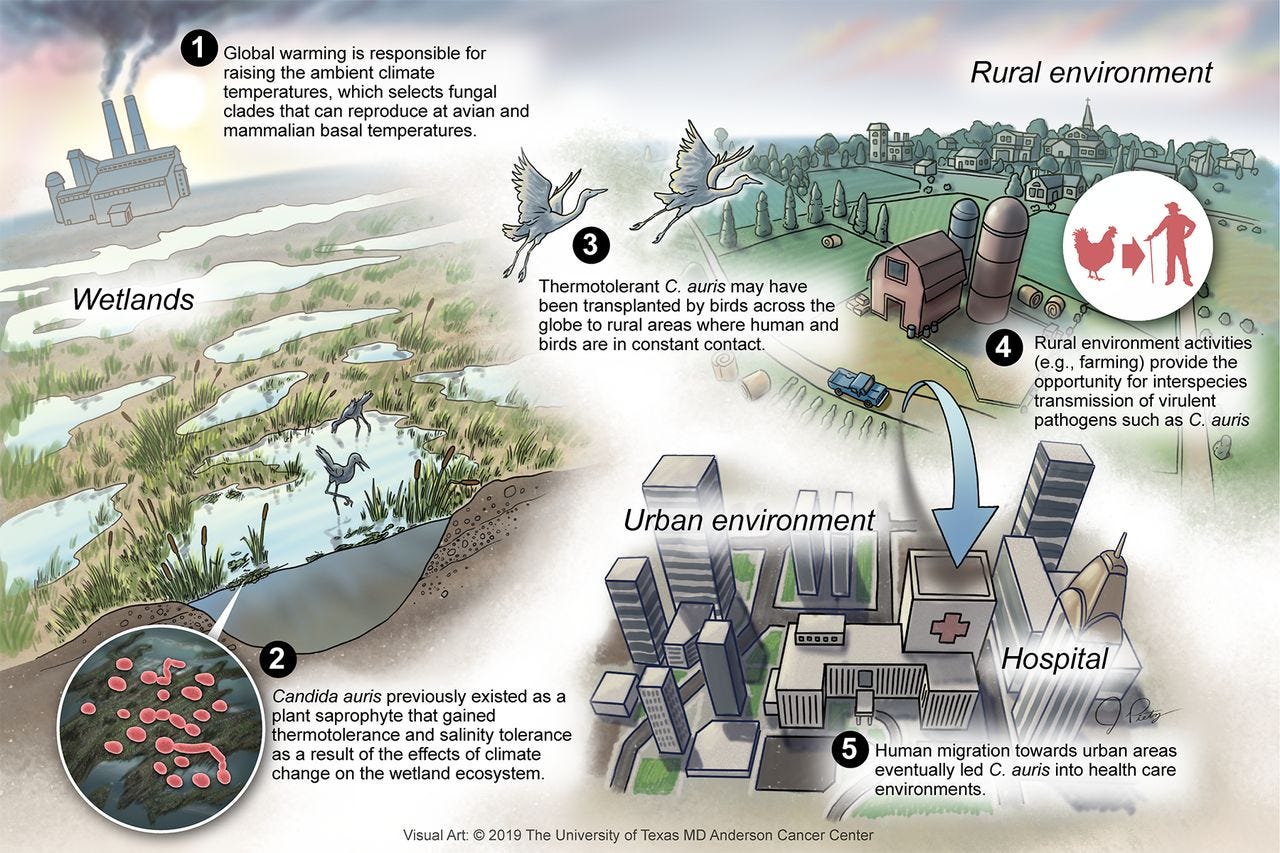
This graphical hypothesis below shows how an environmental bug grows heat-tolerant due to climate change, is moved around by an intermediate host like a bird, colonizes an agricultural area where it becomes anti-fungal resistant and then finally lands in a urban hospital to infect susceptible patients.
How fungal infections have shaped the ecosystem in the past…
If our warm bodies inhibit dangerous fungal infections, then do cooler animals like amphibians get more fungal infections? Absolutely, in fact, many frog species have gone extinct due to fungal outbreaks. The chytrid Batrachochytrium dendrobatidis (Bd) of frogs is considered to be “the most lethal wildlife pathogen in recorded history”.
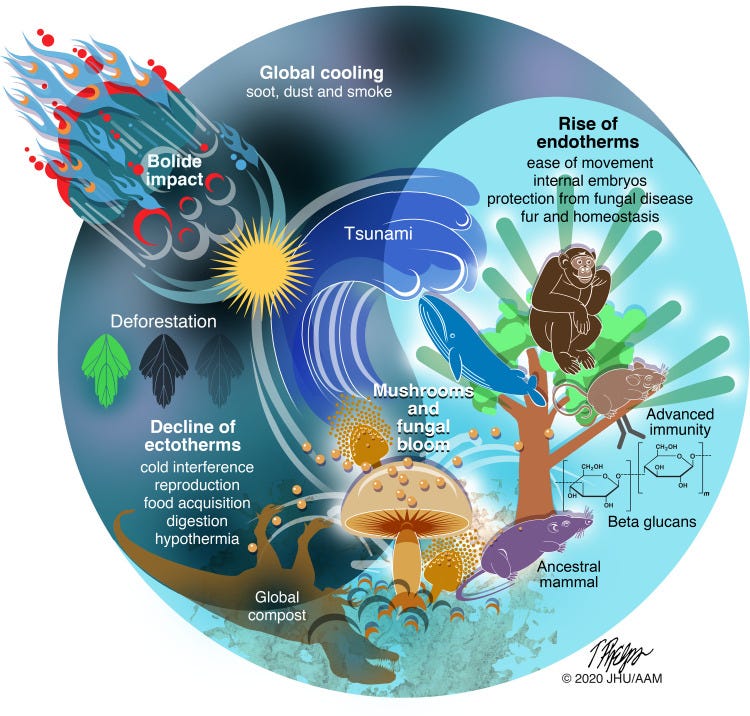
An interesting theory called the Fungal Infection-Mamalian Selection hypothesis (FIMS) states that the reason why mammals are the dominant species on Earth is directly the result of fungal infections. This theory claims that after the worldwide extinction event at the Cretaceous-Tertiary boundary 65 million years ago (probably a bolide meteor hiting the Earth) the Earth cooled, fungal species bloomed, and amphibians (which were once the dominant species) were largely wiped out due to the cooler temperatures and to fungal infections. Mammals became the dominant species because our warm temperatures protected us from those fungal infections.
It seems that species are still being shaped by fungus.
Stay happy, healthy and informed!
Jessica at TCA
General information about Candida auris, CDC.
Spivak and Hanson. Candida auris: an emerging fungal pathogen.
Rossato and Colombo. Candida auris: What Have We Learned About Its Mechanisms of Pathogenicity?
Treatment and Management of C. auris infections and colonization, CDC.
Dix and Webster. Fungi of extreme environments
Casadevall et al. On the Emergence of Candida auris: Climate Change, Azoles, Swamps, and Birds