Florida’s surgeon general uses bad science to write public policy

On October 7, new guidance was released by Governor Ron DeSantis and State Surgeon General Joseph Ladapo, MD/PhD that males aged 18-39 should not receive mRNA based COVID-19 vaccines (Pfizer and Moderna vaccines) because of an increased risk of cardiac death. This guidance is based on bad science. Here is the list of my reasons why, and each issue is expanded on below:
The study is not peer-reviewed, published, or has any authors associated with it.
The number of people studied in the age-groups identified is small (20 people) and its hard to get good statistical power with numbers that small.
Their control group is unusual.
The study uses unusual ways to identify cardiac death
The study does not eliminate those who may have been infected with COVID-19 (which also may increase the risk of cardiac death, confounding their analysis)
The researchers themselves identify severe limitations and flaws in their own study.
(1) The study is not peer-reviewed, published or has any authors associated with it. Here is the study, its literally just a PDF with no authors, names or labs associated with it. I’ve literally never seen such a thing in my entire science-life. The guidance statement says the study was done by the Florida Department of Health, so that’s a start, but we still don’t know who did the study. When studies are published in peer-reviewed journals, they are vetted for validity, accuracy and logic by others in the field. They are analyzed to see if there is any conflict of interests (financial or otherwise) in the researchers. Researchers names are included so that other scientists may contact them for questions, or to ask for details so that the study could be repeated by another lab (this is an INTEGRAL part of the scientific process). None of these things happened here. Why is the Florida Department of Health making sweeping guidance changes based on a anonymous, un-reviewed PDF?
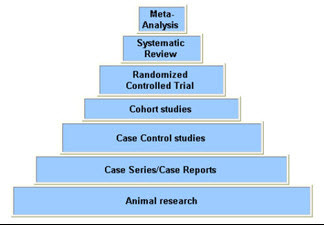
(2) The number of people studied in the age-groups identified is small (20 people) and its hard to get good statistical power with numbers that small. While there are several thousand people in the study, the researchers broke the larger group down into smaller gender- and age-groups and analyzed each group individually. They only found a statistically significant increase in cardiac death in males aged 18-39 who had received a mRNA-based vaccine. That group had 20 people in it. The smaller a group is, the less statistical power you have and the more likely you are to have unrealiable findings. This is a “case-series” type study. Case-series studies are at the bottom in terms of reliability, and have the lowest quality of the different types of human-study designs.
(3) Their control group is unusual. When a good study is looking for adverse events (like death) associated with a vaccine, they look at the rates of those events in vaccinated people and see if its higher or lower than the rates in unvaccinated people. This study compared the rates of cardiac death in vaccinated people right after receiving the vaccine, compared to the SAME PEOPLE 28+ days after receiving the vaccine. So, there is no unvaccinated control. I’ve never seen it done this way. A possible problem here is that vaccines take time to protect you. If you just received a vaccine, you are still susceptible to COVID infection because the vaccine hasn’t “kicked in yet”. COVID infection is associated with cardiac damage. So, an increase in cardiac death in this “just-vaccinated” group could be caused by undetected COVID infection (which wouldn’t happen in the 28+ days after vaccination group, since by then, the vaccine would have protected them from COVID infection). Plus, the researchers didn’t test for COVID in their study (see point 5 below).
(4) The study uses “unusual” ways to identify cardiac death. They identified people who died of cardiac-related reasons by looking through death certificates and pulling out anyone who had an “ICD-10 code of 130-152”. ICD-10 codes are insurance billing codes, and code 130-152 are the codes for “other forms of heart disease”. Again, I have never seen it done this way. These are not actual diagnoses, and the researchers did not go back and confirm that the patients died of cardiac events. They used insurance billing codes (which may or may not be accurate; which may or may not tell the whole story). Good quality studies would have gone back into the medical records themselves and certified that the patient was diagnosed with a cardiac event that led to their death. The researchers themselves state: “the underlying cause of death may not be cardiac-related.”
(5) The study does not eliminate those who may have been infected with COVID-19 (which also may increase the risk of cardiac death, confounding their analysis). Early in the paper, the researchers state: “Individuals were excluded if they (1) had a documented COVID-19 infection, (2) experienced a COVID-19 associated death”. But later in the paper, they say: “This study cannot determine the causative nature of a participant’s death. We used death certificate data and not medical records. COVID testing status was unknown for those who did not die of/with COVID.” So here they state that they did NOT do COVID testing on many of the study participants. COVID-19 infection is known to cause cardiac problems. This is especially important since they are comparing those who had just received COVID vaccines (still might get infected with COVID) to those who had received COVID vaccines 28+ days ago (protected from COVID infection, see point 3 above).
(6) The researchers themselves identify severe limitations and flaws in their own study. The researchers have a LONG list of why this study is flawed. Every study has limitations, but this is a lot. While limitations do not necessarily mean a study is meaningless or invalid, a list of limitations this long should preclude this study from being the SOLE REASON an entire state with a population of 22 million writes a new public health policy.
The Surgeon General, Joseph Ladapo, is no stranger to controversy. He has opposed many guidelines regarding COVID-19, mask mandates, COVID vaccines, and was also a part of America’s Frontline Doctors (a political organization) who promoted unapproved COVID treatments like hydroxychloroquine/ivermectin (off of which they made money).
The HotTake: Florida is using a poorly-designed, anonymously written, and non-published study (with no corroborating back-up studies) to write public health policy and recommend against mRNA-based COVID vaccines for males age 18-39. This is anti-science.
Guidance for mRNA COVID-19 Vaccines October 7, 2022
Colonoscopies May Not Reduce Colon-Cancer Deaths

Colon cancer is the 2nd most common cause of cancer-related death in the United States. Colonoscopies have long been a part of routine screening in adults over 50, however, their ability to reduce cancer death has never been analyzed in a randomized trial until now. (Please note, the following study did NOT include those who have an increased risk of colon cancer. If you have a family history or other predisposing factor, colonoscopies might still be the best choice).
A new randomized clinical trial published in the New England Journal of Medicine reports the results of the “NordiCC study” looking at the rates of colo-rectal cancer, colon-cancer death, or any death, in 84,585 men and women, age 55-64 years old. Half the group was invited to receive a colonoscopy, the other group was not, and just received “usual-care”. They were followed for 10 years. This study was performed in Poland, Norway, Sweeden and the Netherlands where colonoscopies are not a part of routine screenings for healthy adults.
This study found:
Those who were invited to receive colonoscopies had a lower rate of colo-rectal cancer than the control group. Colonoscopies prevented 1 case of cancer for every 455 people who were invited to receive the scans.
There was no statistical difference in the rates of colorectal cancer-death, or any cause of death, between the two groups.
Interesting side note: only 42% of the people invited to receive colonoscopy actually followed through and got the colonoscopy. If they only analyze that subgroup, then they DO see a 31% reduction of colorectal cancer and a 50% reduction in cancer-related death after colonoscopy. However, they cannot remove the possibility that the 42% of those who followed through might have other differences about them: maybe they just take better care of themselves, are more likely to care about their health, or were motivated to get screened because they thought they were at high-risk. Parsing the groups out this way basically “unrandomizes” them and removes the power of randomization in a clinical trial.
The editors of the NEJM summarize this study this way: “This relatively small reduction in the risk of colorectal cancer and the nonsignificant reduction in the risk of death are both surprising and disappointing”.
Its important to note that this study does NOT suggest that people should not get screened for colon cancer, only that colonoscopies may not be the ideal way to screen particularly because of their invasive and budensome nature. Colonoscopies are the gold standard for discovering and removing polyps (the precursor to cancerous growths), identifying 95% of large polyps. However, the preparation for a colonoscopy is intense (having to drink large amounts of fluid and laxatives), the procedure requires anaesthesia (which has its own set of risks), and the patient may have complications like bowel perforation, bleeding, etc.
Considering this new infomation about the limited benefits of colonoscopies, it might be preferrable for low-risk adults to choose another procedure like a flexible sigmoidoscopy, or fecal DNA testing.
Flexible sigmoidoscopy has been shown to also reduce colon cancer incidence and death. While the patient still needs to drink laxatives before, sedation is not required for this procedure. Perhaps this technique is just as effective, but less burdensome, than colonoscopy.
Fecal DNA testing (like Cologuard) is the least invasive or burdensome method of screening. Patients basically “poop in a tube” at home and send the sample to a lab to be tested for abnormal DNA. Cologuard detects 93% of all cancers, but only detects 42% of polyps. Its better at detecting cancer rather than preventing it. But considering its minimally invasive nature, it may be a good choice for routine screening of the low-risk adult.
The HotTake: Colonoscopies are the best technique for detecting and removing pre-cancerous polyps, but new data show that it only slightly reduces the risk of colo-rectal cancer diagnosis and does not prevent death. This information is really important to identify the best screening technique (balancing effectiveness with burden to patient) and some patients may find that flexible sigmoidoscopy or fecal DNA testing is better for their needs.
Effect of Colonoscopy Screening on Risks of Colorectal Death and Related Death
Understanding the Results of a Randomized Trial of Screening Colonoscopy
The truth about Cologuard tests
Stay happy, healthy and informed,
Jessica at The Causative Agent.